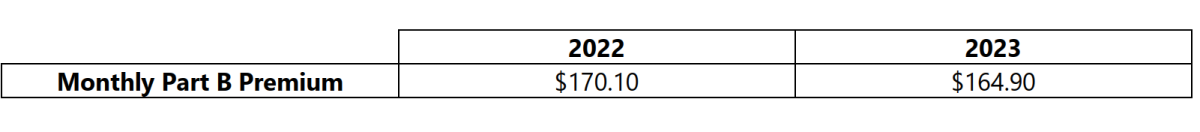Benefits Buzz
Earlier this year, the Centers for Medicare & Medicaid Services (CMS) published some new compliance rules that will impact Third-Party Marketing Organizations (TPMOs) who sell Medicare Advantage and/or Part D plans.
The Internal Revenue Service (IRS) recently published Notice 2022-41 in response to the fixes made to the “family glitch
The Internal Revenue Service (IRS) published Revenue Procedure 2022-38 on October 18, 2022. The Revenue Procedure includes the inflation-adjusted 2023 contribution limits for certain employee benefit programs. Below is a summary of some of those contribution limit adjustments.
Health Flexible Spending Accounts (Health FSAs)
The Department of Treasury published a final regulation on October 13, 2022 which eliminates the so-called “family glitch” starting on January 1, 2023.
Last year, the State of Illinois passed a law called the Consumer Coverage Disclosure Act (CCDA). The CCDA requires a written disclosure to be provided by every employer who has employees in the State of Illinois and who also provides group health insurance coverage to those employees.
On September 27, 2022, the Centers for Medicare & Medicaid Services released the 2023 premiums, deductibles, and coinsurance amounts for the Medicare Part A and Part B programs, and the 2023 Medicare Part D income-related monthly adjustment amounts. Below is a summary of those numbers: