employers
The new reporting requirements that some employers will be subject to starting next year, as required by the Affordable Care Act (ACA), will be used to help the Internal Revenue Service (IRS) enforce the Individual and Employer Mandates, and it will also help the IRS administer subsidy eligibility in the Exchanges.
The following reporting forms will be the responsibility of the employer to complete:

As a trusted benefits administrator, Flexible Benefit Service LLC (Flex) wants to keep you informed on the following:
Federal regulators have recently indicated that they don’t feel the current COBRA notices provide enough information about the Exchanges and the options that COBRA beneficiaries have in the Individual Marketplace.
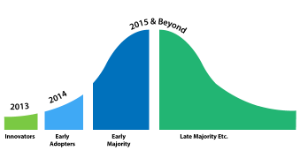
After nearly thirty years of lobbying the “Use-It-or-Lose-It” rule has been changed. Now the option is left to you, the plan sponsor, whether or not it is the right thing to implement for your company. Let’s take a look at some of the scenarios and helpful tips for the healthcare flexible spending account (FSA) rollover option in terms of an adoption lifecycle (a model that shows the trend of acceptance to a new concept over time).
The U.S. Department of Health and Human Services (HHS) released final regulations on March 1, 2013 about the Transitional Reinsurance Program. This new program will require insurance companies and some employers to fund a program that will provide partial reimbursements to commercial insurers that provide coverage to high risk individuals.